King’s student Jasmine Smith, a member of “Universities Allied for Essential Medicines”, explains how rich nations including the United Kingdom are preventing the developing world from accessing vital Coronavirus vaccinesÂ
In December 2020, the world’s first Covid-19 vaccine rollout began in the United Kingdom. Since then, many more countries have begun their own vaccine programmes. As of March 2021, Europe, the United States, and the UK have administered between 13 and 23 doses per 100 people. However, some low and middle-income countries (LMICs) have yet to administer even one, with Africa and Asia administering between 0.6 and 3.8 doses per 100 people according to the New York Times. In order to maximise the vaccine rollout globally, LMICs need to have the right to produce the relevant health technologies. Unfortunately, the agreement on Trade-Related Aspects of Intellectual Property Rights (TRIPS) means this is impossible.
In response to the crisis, 57 LMICs have co-sponsored a waiver for Covid-related health technology. However, it is those high-income countries that already have extensive vaccination programmes, such as the United Kingdom and the United States, that have the vote that matters, and for now, they remain against waiving the patent rights to improve access to these health technologies, which are especially important for Covid-19 vaccines.
The proposal, originally put forward by South Africa and India in October 2020, is calling for a temporary suspension of the intellectual property protections over the vaccines being created by pharmaceutical companies such as Pfizer, AstraZeneca, and Moderna. The patents currently in place grant the sole rights of licensing for vaccine production to the companies that originally made the vaccine, for 20 years. This means that pharmaceutical companies control the market for these vaccines, preventing generic and therefore cheaper versions from being made which would improve access for LMICs.
But why is this a problem? For many LMICs, the prices that are set by pharmaceutical companies are unaffordable. Furthermore, high-income countries like the UK were able to make bilateral trade agreements with these companies to agree on cheaper purchasing prices. The countries calling for the waiver do not have those agreements in place. Many lack purchasing power, meaning they have little influence over the market prices.
However, for almost all LMICs, a reliance on subsidised vaccines through the COVAX, a World Health Organisation programme to provide healthcare to LMICs, has resulted in delays in rollout and limited vaccine supplies. This results in varying prices for each country. For example, the UK is paying the US $3.50 per dose for the Modern vaccine while Uganda is paying $8.50. There are many more cases of exponential price differences, which calls into question the claim that high-income countries such as the UK are “driving forward efforts to ensure equitable accessâ€. Waiving TRIPS would allow countries like Uganda to get more involved with vaccine production, rebalancing the traditional state of affairs in which high-income countries produce and low-income countries are given or buy, ultimately providing cheaper, generic versions of these life-saving vaccines.
The benefits of the TRIPS waiver do not just correlate to benefits for LMICs. £6.6 trillion is the predicted cost to the global economy for delays to vaccine access in poorer nations. Nearly half of this cost will be taken on by richer nations, such as the UK and the US. By improving access for all through granting the TRIPS waiver, high-income countries therefore will see long-term economic benefits. However, doubt continues surrounding the abilities of the vaccine to defend against new variants. A consequence of not efficiently vaccinating a substantial percentage of the global population is that the disease gets an opportunity to mutate, an opportunity it will not fail to take up. Undoubtedly, these mutations will travel the world with globalisation, and eventually, make it to the shores of the vaccinated. This is preventable with the increased vaccine access to low-income countries.
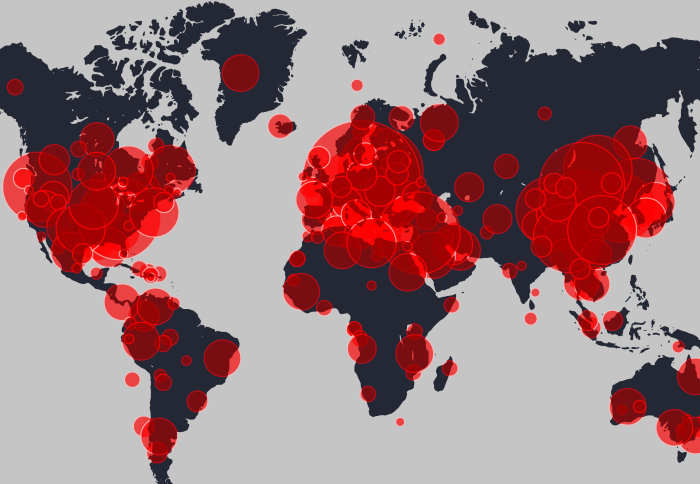
A map by “Doctors without Borders” shows where countries across the world currently stand on support of the waiver. There is a stark difference in the position of affluent, developed nations and poorer ones.
The World Trade Organisation has held multiple meetings since the waiver was first proposed. In February 2021, the TRIPs Council met once again to discuss the waiver, with the outcome facing continued blockage from the US, UK, EU, Japan, and Australia. Why are they blocking it? Well, these countries are claiming that there is already enough flexibility within the TRIPs agreement through compulsory licensing to allow for these supporting countries to improve access to the vaccine. They also claim that the patents themselves are not the issue with the accessibility of the drug, but rather a lack of production capacity to meet the needs of the global population. As a result, high-income countries argue that there is little reason to grant the waiver.
The issue with these claims is that although compulsory licensing, to a degree, does grant some flexibilities within the TRIPS agreement, it also requires countries that utilise it to pay the rights holder a fee, which in the current climate may be detrimental to economies that have been hardest hit by the pandemic according to Exeter University. Moreover, if the issue, as they say, is to do with the ability of these companies to produce the vaccine at a fast enough rate to meet demand, then there is no reason not to grant the patent waiver and allow countries around the world to produce generics to enable faster production and bring an end to this pandemic.
The prevention of the waiver, coined as “vaccine apartheid” by Dr. Thabo Makgoba, the archbishop of Cape Town, is costing millions of lives around the world. The hypocrisy of high-income countries, such as the UK (Britain spent three times the amount of the their vaccine programme on the failed track and trace scheme), who claim to be supportive of programmes improving accessibility to LMICs but are blocking this waiver shows the world how much work there is to do. Organisations such as Global Justice Now, alongside Universities Allied for Essential Medicines (UAEM), are campaigning for countries to support the TRIPS waiver through raising awareness and encouraging people to support the cause through signing their petition and putting pressure on the UK government. Combining the work of these organisations with the 100+ countries supporting the TRIPs waiver, the world is demanding resolutions for the question we are all asking, where is the vaccine?
To take action or find out more about the campaign to end restrictive Covid-19 vaccine patents visit “Global Justice Now” here.
Jasmine Smith